THE KNEE
MENISCUS INJURIES
There are two menisci in your knee, a medial (inner) and a lateral (outer). They are circular structures made of cartilage – a different type that covers the ends of bones that form joints. They are commonly known as shock absorbers, but they serve an important stabilization function as well. Thus, the preservation of their structure and function is very important to protect the other cartilage in your knee, prevent degeneration and optimize function.
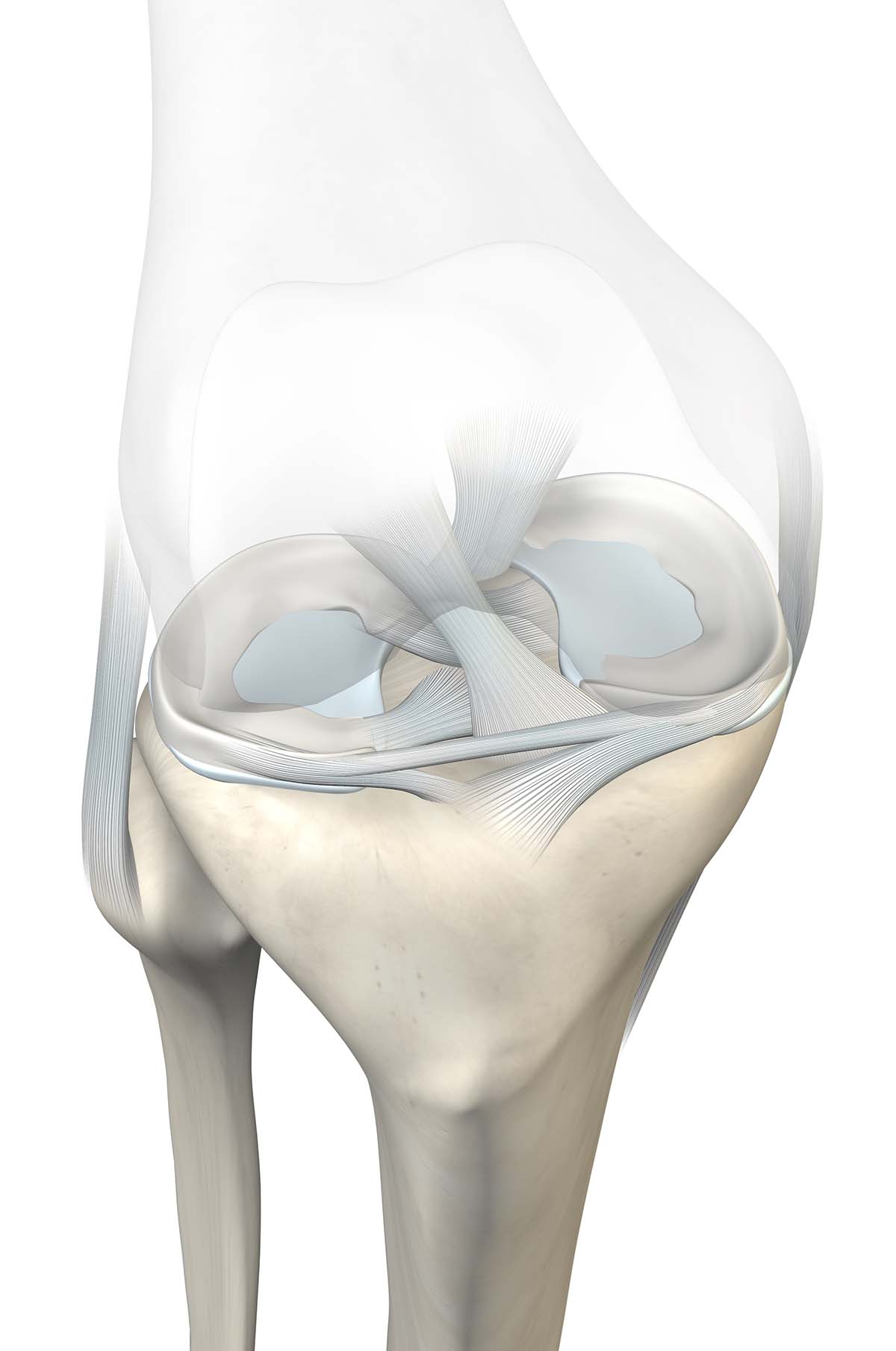
A Special Word on Meniscus Transplantation
Through injury, neglect of an injury, prior surgery or other circumstances some younger patients may be left with very little meniscus. While this may be unavoidable, in the right hands, it may be manageable.
In the past these patients were doomed to very early degeneration of the knee. This left very few treatment options and little hope for a highly functional knee at a young age. In the right patient, a cadaveric meniscus graft can be used to substitute for a significant meniscus deficiency. In these instances, I will perform a thorough assessment of your lower extremity (Hip, knee and ankle) alignment. It is not uncommon we must perform an additional realignment surgery to protect the meniscus graft. This can be a complex, multi-stage treatment plan and often is combined with ACL reconstruction and realignment osteotomies. Given the complexity of the injury and surgical management, seeking out an ACGME accredited fellowship trained sports surgeon is imperative.
Causes
Injury to the meniscus is the most common indication for arthroscopic knee surgery. Meniscal injury can result from an acute injury (very commonly seen with ACL tears) or from a slower, degenerative process.
Symptoms
Regardless of the cause, if meniscal injury is causing your knee to swell, lock, catch or give way – collectively known as mechanical symptoms – we need to evaluate your knee and design a treatment plan tailored to your personal goals.
Diagnosis
For patients experiencing symptoms physical examination in the office diagnoses most injuries, however a detailed history is as important to help determine severity. We will obtain advanced imaging to further assess the injury and guide the next steps in treatment.
Non-Operative Treatment
If you are not experiencing the above mechanical symptoms, we will undoubtedly attempt to resolve your complaints with a thorough course of non-operative management. This would involve a combination of a brief course of oral anti-inflammatories, activity modifications, injections, physical therapy, and home exercise and, if applicable, a return to sport plan.
If this management fails, then we discuss further options. Typically, this will be a more invasive option.
Operative Treatment
Even if mechanical symptoms are present, I may recommend an attempted course of nonoperative management in some cases.
If we decide upon surgical management, the options are to repair or resect (shave out). Why not repair everything you may ask? Well, in order for a repair to heal, we must have the biology present to support it. The meniscus does not have a robust blood supply. Thus, if the tear is in an area with poor blood supply or if it is a degenerative tear, healing of an attempted repair is unlikely and I will resect only what is necessary to remove the offending tissue.
Evidence over the last few decades strongly supports saving the meniscus whenever possible, thus every attempt is made to do so.
Meniscal Repair
Rehabilitation is tailored to maximize the protection of the repair. You will be in a hinged knee brace, locked straight in extension while putting any weight on your leg, for a total of 6 weeks. When you are not putting weight on your knee, you will unlock your brace and perform a range of motion exercises. I provide a detailed rehabilitation protocol for you and your therapist to follow. A very general expectation is to return to sport no sooner than 6 months, but again this varies with every individual.
Meniscal Resection aka “Meniscectomy”. This indicates no healing was expected and I shaved out only the amount of meniscus necessary to stabilize the tear and remove only the offending tissue. In this case you will not need a brace and can resume normal activity as soon as your pain and swelling resolve. As always, however, I will want you to follow a structured rehabilitation plan.
The Knee
Cartilage AKA Chondral Injuries
Cartilage comes in many forms. Here we are talking about the type of cartilage that covers bones that forms a joint. For those interested, this is Type II or Hyaline Cartilage. Have you ever seen the shiny, smooth end of a chicken bone? That is what we are talking about here.
The cartilage injuries we manage in the sports surgery world are different than the more widespread degeneration of cartilage otherwise known as osteoarthritis. Here we are talking of more localized injuries akin to “potholes” in your cartilage. These can come in many sizes and shapes and thus treatment options are many.
Causes
Cartilage injuries can occur in the same manner as meniscal or ligament injuries to the knee. A pivoting or twisting motion, an awkward landing from a jump or even direct trauma can result in an acute (sudden) injury to your cartilage.
Symptoms
Symptoms can mimic those of ligament and meniscal injuries. Knee pain, swelling, catching, locking and giving way are common complaints.
Diagnosis
For patients experiencing symptoms physical examination in the office diagnoses most injuries, however, a detailed history is as important to help determine severity. We will obtain advanced imaging to further assess the injury and guide the next steps in treatment.
Non-Operative Treatment
Not all cartilage injuries will require surgery. If the lesion is small and thus likely stable and you are not suffering from mechanical symptoms such as swelling, locking, catching, or giving way nonoperative is a good option. We will focus on the reduction of pain and swelling and strengthening by a dedicated physical therapy and home exercise program.
Operative Treatment
If the lesion is large and producing mechanical symptoms such as swelling, giving way, locking, and/or catching we will discuss surgical management.
There are many ways to manage these injuries and they must be individualized to the patient goals and lesion characteristics. In general, smaller lesions can be managed with an arthroscopic only approach. Larger lesions, however, will typically require a combination of arthroscopic and open surgery. These can involve grafts taken composed of bone plugs with cartilage caps taken from areas of your knee which do not see much pressure or similar grafts from a cadaver donor. Larger lesions are managed with cadaver grafts as using grafts from your own knee is not ideal, to say the least.
Cartilage defects on the undersurface of the patella (“knee-cap”) deserve special mention. It is not uncommon these lesions exist in the setting of poor knee alignment. We will fully evaluate the alignment of your entire lower extremity (thigh and leg) to determine if a realignment surgery is also necessary. In many cases, alignment is not properly assessed thus dooming your surgery to fail.
What to Expect After Surgery
Surgery will be done as an outpatient or “Same Day.”
A bracing and protected weight-bearing period of AT LEAST 8 weeks after surgery is nearly universal in my practice. Additionally, I will only allow a range of motion of the knee when it is unloaded, that is no weight is being placed on it. This serves to protect the graft from excessive pressure and force that will hinder healing.
During the first 8 weeks, you will work closely with a physical therapist to reduce swelling, pain and regain your range of motion. After 8 weeks we will sequentially progress through a dedicated strengthening and return to sport protocol.
Return to sport timelines vary widely from 3 months to 6+ months and thus we will discuss this on an individual basis.
The Knee
Anterior Cruciate Ligament Injuries
The Anterior Cruciate Ligament (aka “ACL”) is a very common reason for patients to undergo surgery. This ligament prevents abnormal rotation and translation (back and forth movement) of your knee. For patients wishing to return to activities that require cutting, pivoting, or side to side movements you become a candidate for ACL repair or reconstruction. Without treatment, we know ACL deficiency leads to increased damage to the menisci and cartilage of the knee which can significantly limit your function and activities.
Causes
ACL injuries typically occur from an awkward and forceful twisting motion at your knee. Rarely do they occur from direct contact or a direct blow, but they can occur with high-energy trauma (a car accident for example).
Symptoms
Patients commonly experience a “pop” sensation or sound – I know I did with my ACL tear – at the time of injury. A few hours later the knee will swell and pain will begin, the amount will vary between individuals. If left to go without evaluation and treatment patients will sense their knee is less stable, less trustworthy with side to side or pivoting motions.
Diagnosis
Physical examination in the office diagnoses most injuries, however, a detailed history is as important to help determine severity. MRI is especially helpful to determine the grade of injury but typically will only be obtained if there is concern surgery is needed.
Do not let an outside practitioner tell you you are “too old” for an ACL reconstruction. Recent evidence has shown patients once thought to be “too old” are indeed candidates. While this is not universally true if you are youthful, active, healthy and without significant arthritis, ACL reconstruction or repair may be a good option.
Non-Operative Treatment
Is it possible to live without an ACL? Of course, it is. For some patients who do not have high demands on their knee or do not wish to undergo surgery and rigorous postoperative rehabilitation, this may be a good option. What we do know, however, is without an ACL the biomechanics of your knee are different. This leads to an increased risk of meniscal tears, and, more importantly, early degenerative changes.
Operative Treatment
Operative treatment, as with most things, comes into play when non-operative management fails to achieve your goals. I typically perform tendon repair thru a mini-open approach, but still as a same-day or outpatient procedure.
ACL Repair
What was once a very criticized treatment has undergone a resurgence. Why? A recent analysis of historical data has shown in specific tear types, ACL repair to its bony insertion on the femur (thigh bone) do very well. Repairs can decrease pain and difficulty in the postoperative setting as we do not need to take a tendon graft from elsewhere in the knee. While data is still emerging as to if ACL Repairs can reliably return patients to normal activity or sports faster, I do know after my ACL Reconstruction the graft harvest site was very painful. If I can make your postoperative period easier I will. It is important to note you must be a candidate for Repair, only certain tear types are candidates. We will discuss this at your visit. There are few practitioners trained in this procedure.
ACL Reconstruction
Reconstruction with another tendon – from elsewhere in your own knee aka “Autograft” or that of a cadaver donor “Allograft” – remains the gold standard for most ACL tear types. The founder of my fellowship played a large part in the development of the All-Inside technique using a quadriceps tendon which is becoming popular today. This is my technique of choice. Why? The quadriceps tendon provides a strong, linear, graft which has been shown to remodel resembling a normal ACL in “second look” studies.
The other classic grafts – hamstring and patellar tendon- are not without drawbacks. The patellar tendon graft certainly has benefits but is notorious for producing anterior knee pain and pain with kneeling. The hamstring tendon, in its normal function, is a stabilizer of the knee in the same way a normal ACL performs by preventing anterior (forward) translation of the tibia (your shin bone). By preserving the hamstring, I preserve a stabilizer of the knee which is protective of your ACL reconstruction. Further, in certain populations, hamstring weakness is associated with poor knee biomechanics leading to an increased risk of ACL rupture or re-rupture.
If I could do it all over again, I would have a quadriceps tendon ACL reconstruction. As a general rule, I will not recommend a treatment option I would not recommend to my own family members.
Preparing for Surgery
It is important to note there is no graft nor technique proven in the scientific literature to reliably reduce the time it takes to return to sport. Beware of claims promising a technique or graft will result in an earlier return to sport or activity, they are not founded in current evidence nor science. Only a combination of well-executed surgery with modern techniques and dedication to physical therapy and hard work can guarantee a successful result.
Weaks Leading Up to Surgery
You will meet with a physical therapist to ensure you have a full range of motion before undergoing surgery. This is of crucial importance to insure you can achieve a full range of motion after surgery. You will also learn the exercises I want you to do immediately before surgery. Finally, preoperative appointments make obtaining timely postoperative appointments much easier.
We will meet and review your personal goals and the surgical goals, risks, alternatives, and postoperative rehabilitation timeline. Additionally, we will make sure all your needs are in place: Braces, crutches, pain meds, medical evaluation (if necessary), etc.
Day of Surgery
Surgery is done on a same-day or outpatient basis. You will be provided with an immediate postoperative brace, detailed postoperative instructions in writing, your physical therapy protocol, and postoperative pain management instructions. Ideally, we will have had a preoperative visit where you received a prescription for pain medication and to ensure all bracing/crutches, medical evaluation, labs, etc. are in place.
What to Expect After of Surgery
Weeks 0-6
This time is dedicated to swelling and pain reduction and regaining your full range of motion. I will see you within 14 days of your surgery
You will wear your immediate postoperative brace locked in extension until you are able to perform a straight leg raise (Typically, this takes 2-3 weeks)
Weeks 7-12
Gentle strengthening begins
Full Range of Motion must be achieved by Week 12 after surgery
Weeks 17-20
Jogging commences in all if not already done so
Plyometric exercises introduced
Continued core and lower extremity strengthening
Weeks 21-24
Sport-specific mechanics and form are fine-tuned
Continue all above
Weeks 25+
Dynamic strength assessment for return to sport and full activities is performed in our office visit
If inadequate stability and strength of the knee are found then all of the above continues and we reassess at 4-week intervals.
The Knee
Medial Collateral Ligament Injuries
The medial collateral ligament (aka MCL) prevents the knee from buckling inward – think of the “knock-kneed” position. As you will see with other knee structures, the MCL also plays a role in stabilizing the knee to rotational and translational (front-to-back movement) forces.
Causes
MCL injuries are the most common ligamentous knee injury. It is usually an isolated injury but is known to also occur with an ACL injury. If these two occur together it is termed a “Multi Ligamentous Knee Injury” and should be managed by an ACGME accredited fellowship-trained surgeon. Patients may suffer this injury either from an awkward twisting knee injury or from a direct blow to the outside of the knee.
Symptoms
Pain will occur along the inside of the knee. An MCL injury itself may not lead to knee swelling as this structure is outside the knee joint. If left untreated gross knee instability will persist limiting high-demand activities into the future.
Diagnosis
For patients experiencing symptoms physical examination in the office diagnoses most injuries, however, a detailed history is as important to help determine severity. We will obtain advanced imaging to further assess the injury and guide the next steps in treatment.
Non-Operative Treatment
The vast majority of MCL injuries can be treated nonoperatively with a period of bracing and physical therapy. Because this ligament is outside the knee it has the capacity to heal on its own. ACL injuries are not afforded this luxury as the thick joint fluid (aka synovial fluid) does not allow the torn ends to heal back to themselves.
Operative Treatment
MCL injuries involving the tibial (shin bone) insertion are less likely to heal on their own. This is due to the anatomy of the insertion, where the torn ends flip over nearby structures and cannot contact their bony insertion to heal to it.
If involved in a “multi-ligamentous” knee injury I am more likely to reconstruct or repair the ligament to ensure your knee is stable during the rehabilitation of the other repaired or reconstructed knee structures.
If possible, I will repair your own tissues. If the tear is unlikely to heal with the repair I will likely use a cadaver tendon (allograft) to reconstruct the damaged ligament.
What to Expect After Surgery
For nonoperative treatment, you will undergo a period of bracing and controlled range of motion, the length of which varies based on injury severity.
If operative treatment is indicated you can expect this bracing and controlled range of motion period to be approximately 6 weeks.
It is important to note you will be able to put weight on your leg during this time, but will likely require the assistance of crutches for ambulation.
The Knee
Lateral, Collateral Ligament, and Posterolateral Corner Injuries
The Lateral Collateral Ligament aka “LCL” is a part of the Posterolateral Corner Complex aka “PLC” which are structures on the outer aspect of your knee which control outward bowing (as in bow-legged position) and external rotation of your knee. The LCL and PLC are only rarely injured in isolation. If they are injured, I always suspect further structures to be injured.
Causes
These injuries can occur from awkward twisting injuries, a direct blow to the inner aspect of the knee, or from higher energy trauma.
Symptoms
You will experience pain on the outer aspect of the knee often with going up and down stairs, if part of a multi-ligamentous knee injury swelling can occur, additionally patients will experience a sensation of instability and you may feel your knee thrusts outward during walking or more strenuous activities.
Diagnosis
Injuries to the PLC often are missed and if not addressed can compromise attempts at treating the other damaged structures of the knee. These can be highly complex injuries. This underscores the importance of being seen by a practitioner who has completed an (ACGME) accredited fellowship in sports surgery.
Non-Operative Treatment
For minor sprains and partial tears of the LCL we can manage the injury with physical therapy, bracing and protected movements. In these relatively less common scenarios, we can reliably expect a return to sport or activity in 6-8 weeks.
Operative Treatment
For complete tears of the LCL- especially if the bony insertion from the fibula (small bone in the leg beneath the knee) is pulled off (aka avulsion injury), injuries to the PLC causing instability or a multi-ligamentous knee injury, surgical intervention is discussed.
If there is an avulsion injury of the LCL attachment to the fibula we do not delay in attempting to repair this as we would with any fracture.
If there is a complete tear of the LCL with associated instability or further involvement of the PLC in the setting of a multi-ligamentous injury we commonly discuss reconstruction as a part of a staged procedure to address all injuries. The details of which we will discuss at your visit. Graft choices in these situations can be another tendon about the knee (autograft) or that of a cadaver (allograft), depending on the extent of your injury.
What to Expect After Surgery
If in the rare instance, we repair or reconstruct only the LCL, you will undergo a period of bracing and protected range of motion for approximately 6 weeks. After this, we will advance your physical therapy with an anticipated return to sport or normal activity in 3 months.
In the more common setting where LCL/PLC injuries require surgery, we are dealing with a multi-ligamentous knee injury which can be quite complex. Commonly I will stage the treatment of these injuries. These injuries can be extensive and are highly individualized, thus any expectations of rehabilitation time and return to activity must be discussed on an individual basis. Again, in these instances, it is imperative to seek treatment from a highly trained specialist. Preferably one who has completed an ACGME accredited sports surgery fellowship.
The Knee
Posterior Cruciate Ligament Injuries
The posterior cruciate ligament, aka PCL, is the counterpart to the more commonly known ACL (anterior cruciate ligament). Its main function is to prevent posterior (backward) movement of the tibia (shin bone). In a smaller, although still important, role it helps prevent external rotation and varus (think bow-legged position) forces at the knee. The classic mechanism of injury is during car accidents when the knee strikes the dashboard. Alternatively, sports injuries can occur during knee hyperextension or when the knee is flexed 90 degrees with the ankle pointed down (plantarflexed).
Causes
PCL injuries can occur in isolation. However, they are common components of a multi-ligamentous knee injury.
Diagnosis
If the PCL is injured, I will look extensively for an additional injury to the knee, especially to the Posterolateral ligamentous complex (aka PLC – see above section).
Non-Operative Treatment
Not all PCL injuries require surgery. As with all knee injuries, we will discuss the nature of your injury and your treatment goals. Together we will come to a decision as to your treatment protocol.
In general, for those who are less active, the knee is stable, and/or there are no further injuries to the knee we will discuss a period of bracing and physical therapy.
Operative Treatment
For those patients with complete PCL injuries, knee instability, and those whose PCL injury is part of complex multi-ligamentous injuries we discuss surgical intervention. If initial non-operative management fails and the knee still feels unstable, we will also discuss surgery. In special circumstances, a piece of bone is pulled off the tibial insertion of the ligament. If this occurs, we discuss surgery on a more urgent basis as we would with any fracture scenario.
PCL Repair/Bony Avulsion Repair
If a piece of bone is pulled off the tibial (shin bone) insertion of the PCL we repair it back down to its insertion site. Unlike the ACL we do not typically repair the PCL unless a piece of bone is pulled off the tibia.
PCL Reconstruction
In the event of persistent instability after nonoperative management or complete tears with knee instability after an isolated PCL tear, we will discuss PCL reconstruction. This can be done with your own tissue by harvesting another tendon from elsewhere in the knee (autograft) or from a cadaver donor (allograft). We will discuss the pros and cons of both as necessary.
In the event, a PCL injury is part of a larger, more complex multi-ligamentous injury we will reconstruct the PCL most likely with a cadaver donor tendon (allograft). This will be done in a staged manner, most likely at the time of ACL reconstruction. This is a highly complex and individualized injury with several variations requiring individualized treatment approaches. Given the degree of complexity, I recommend these injuries be managed by a surgeon who has completed an ACGME accredited Sports Surgery Fellowship.
What to Expect After Surgery
Similar to ACL injuries you will undergo a period of bracing and early measures directed at reducing swelling, pain and achieving full range of motion. Restrictions will differ from those of the more common ACL surgery although the overall timeline may be similar. You will work closely with me and your physical therapy team to maximize core and especially quadriceps strength over a period of months. A return to sport should not be expected earlier than 6 months postoperatively.
As with ACL surgery, no graft nor technique has been proven in the scientific literature to accelerate return to sport and activity. Beware of claims to the contrary. Only a combination of well-executed surgery, hard work, and a dedication to physical therapy can guarantee a successful result.